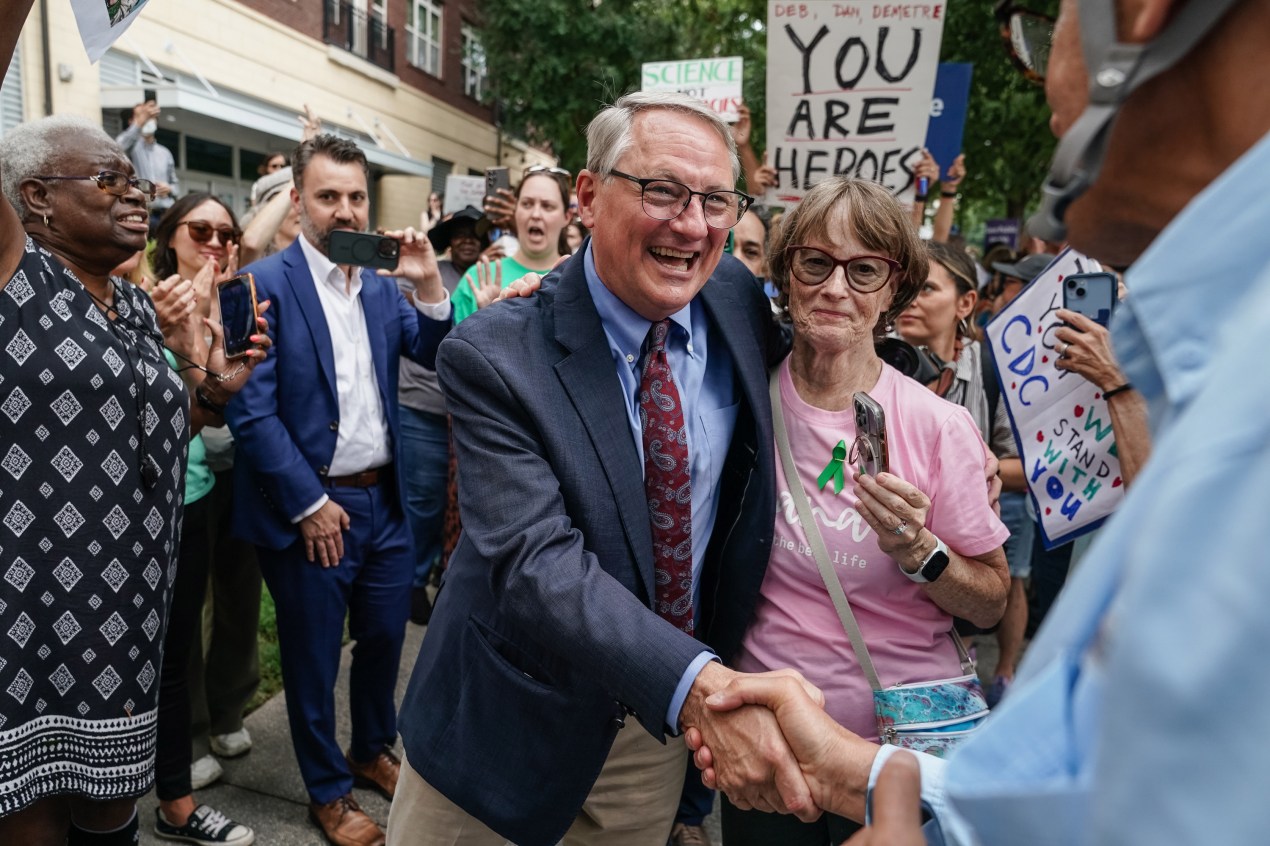SALT LAKE CITY — Ben Dowse hadn’t expected to treat measles when he became a doctor, but there he was, examining a newborn exposed to the virus in the womb. The infected mother had given birth just hours earlier. The hospital had alerted Dowse to the case before delivery, and he’d braced himself for the worst.
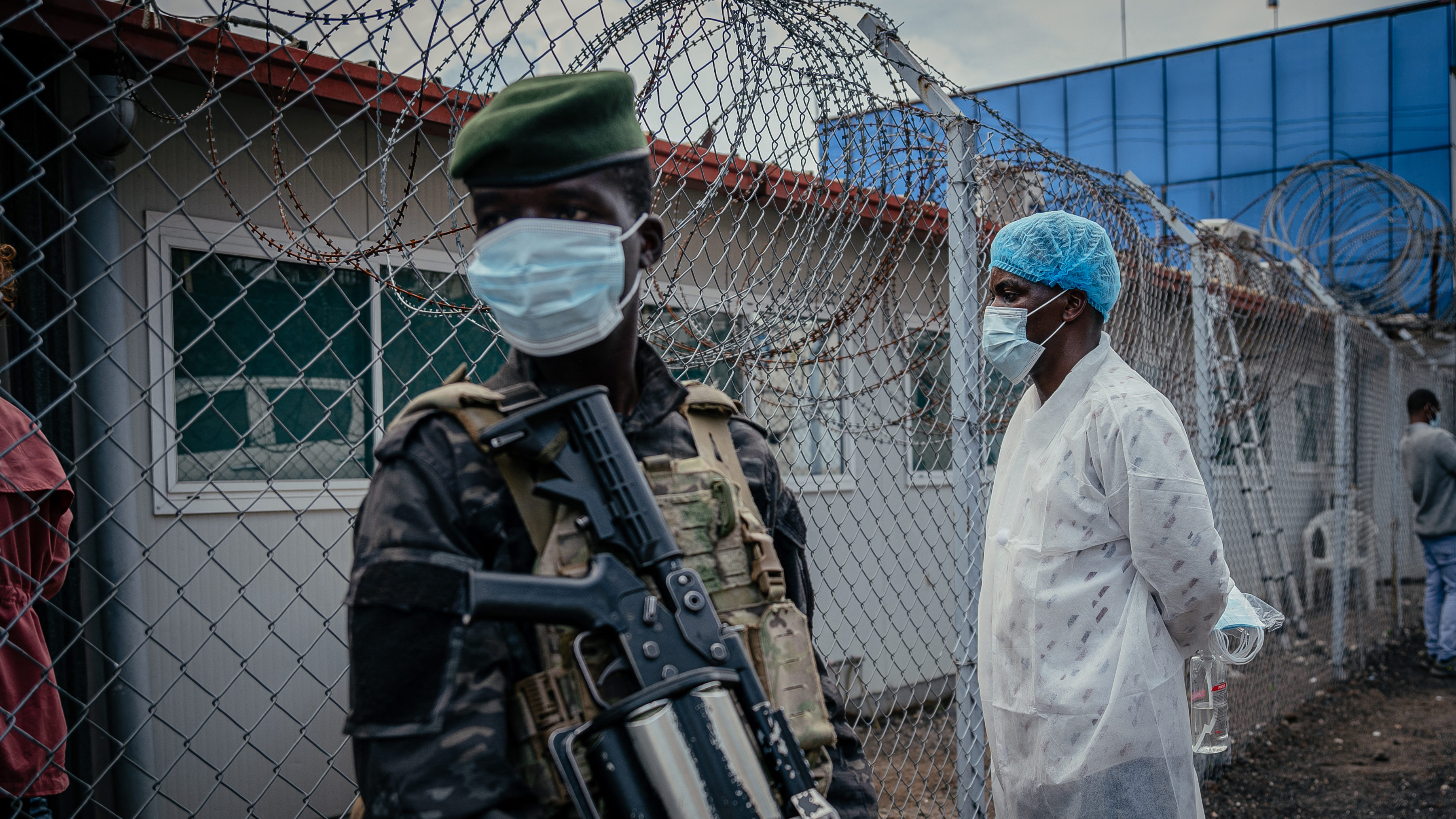
Dowse wore a full-body protective suit with a plastic face mask. As a pediatrician in southern Utah, he couldn’t risk getting even a mild infection, because many of his patients are babies too young for measles vaccines or children whose parents choose not to protect them with immunizations. “I went in looking like a scientist in E.T.,” he said.
Measles can cause brain damage, deafness, or death in newborns. If the baby entered the world with a measles rash and fever, Dowse was prepared to give the infant a spinal tap to assess the risk of neurological damage.
Luckily, flushed and crying, the baby looked healthy. To keep it that way, Dowse wanted to inject the baby with concentrated antibodies against the measles virus. To his surprise, the parents objected, promising to give their child “all kinds of vitamin A,” Dowse said. He begged them not to, saying, “You can’t see it on the surface, but the baby’s body is fighting the measles.” They were afraid of vaccines, so Dowse explained that antibodies were different and that they would stop measles from replicating in the infant.
“That shot is going to basically give the baby ammo to fight,” Dowse said.
The parents relented. A couple of days later, they left the hospital with a child who had narrowly skirted an infection that killed many thousands of babies a century ago. Nonetheless, Dowse said he doubted they would be returning for childhood vaccinations to protect their baby against a bevy of illnesses. Like more than a dozen Utah doctors and health officials who spoke with KFF Health News, Dowse has adjusted his expectations.
He is part of a reluctant cohort of medical professionals now on the front line of America’s regressive next chapter in health history, one in which dangerous and preventable diseases return.
“I wish that people could see what I see,” said Nathan Money, a hospital pediatrician in Utah whose eyes welled up with tears as he described children he’s treated for measles struggling to breathe. “This train is going in the wrong direction, and it can feel like a helpless situation, because we’re just not seeing the public messaging and leadership that’s needed to turn this around.”
Since measles was deemed eliminated in the U.S. a quarter century ago, public health workers have extinguished sporadic outbreaks in close-knit, undervaccinated communities with targeted methods: Isolate people with measles and quarantine their contacts to contain the virus. But as vaccination rates drop nationwide, the virus is moving beyond insulated communities, overwhelming public health departments constrained by shoestring budgets. Larger outbreaks, the kind not seen for a generation, have forced health officials into a new paradigm: They have stopped racing to “contain” infections and shifted gears into what they call “mitigation.”
Utah made that transition early this year, once the outbreak hit “a point where you no longer have control over it,” said state epidemiologist Leisha Nolen. By March, measles had been detected in every health jurisdiction in the state and in northern Arizona. More than 950 people have tested positive in the two states since the outbreak began in August, but many people with measles haven’t been tested. A genetic analysis of measles viruses suggested that the true number of cases last year could have been 6.5 times what was known.
Last year under President Donald Trump, U.S. measles cases exceeded 2,000 for the first time since 1992. Six months into 2026, the U.S. has already surpassed that threshold. Prolonged outbreaks exact a toll on children, who have spent days in hospitals for severe infections and missed weeks of school for mild ones. Adults with measles miss work. Parents delay daycare to keep their babies safe. Doctors in Utah have enacted labor-intensive protocols to keep measles from spreading in clinics. Newborns and people with weakened immune systems who have been exposed to the virus receive infusions of concentrated antibodies costing $500 to $1,000. Medical visits for measles can cost more than $33,000 per patient. Health departments spend millions trying to curb infections.

“This is like a snowball that gathers speed as it rolls downhill,” said Emilie Morris, a hospital pediatrician in Salt Lake County and Utah County. A full-throttle campaign to educate communities on the safety of vaccines and the diseases they prevent could turn the situation around, doctors and health officials said. It would require an effort similar to what the anti-vaccine movement has long done in videos, blogs, and podcasts. For example, the anti-vaccine organization that Robert F. Kennedy Jr. founded before taking the helm at the Department of Health and Human Services, Children’s Health Defense, visits vaccine-hesitant communities, produces movies, and has bought advertisements on Facebook that downplay the threat of viruses while wildly exaggerating the risk of vaccine side effects. Kennedy’s words and actions as health secretary are adding to parents’ doubt.
After the development of vaccines and antibiotics in the mid-1900s, virologist and Nobel laureate Frank Macfarlane Burnet wrote, “One can think of the middle of the twentieth century as the end of one of the most important social revolutions in history, the virtual elimination of the infectious diseases as a significant factor in social life.”
He couldn’t have imagined what was coming.
‘Year of Sickness’

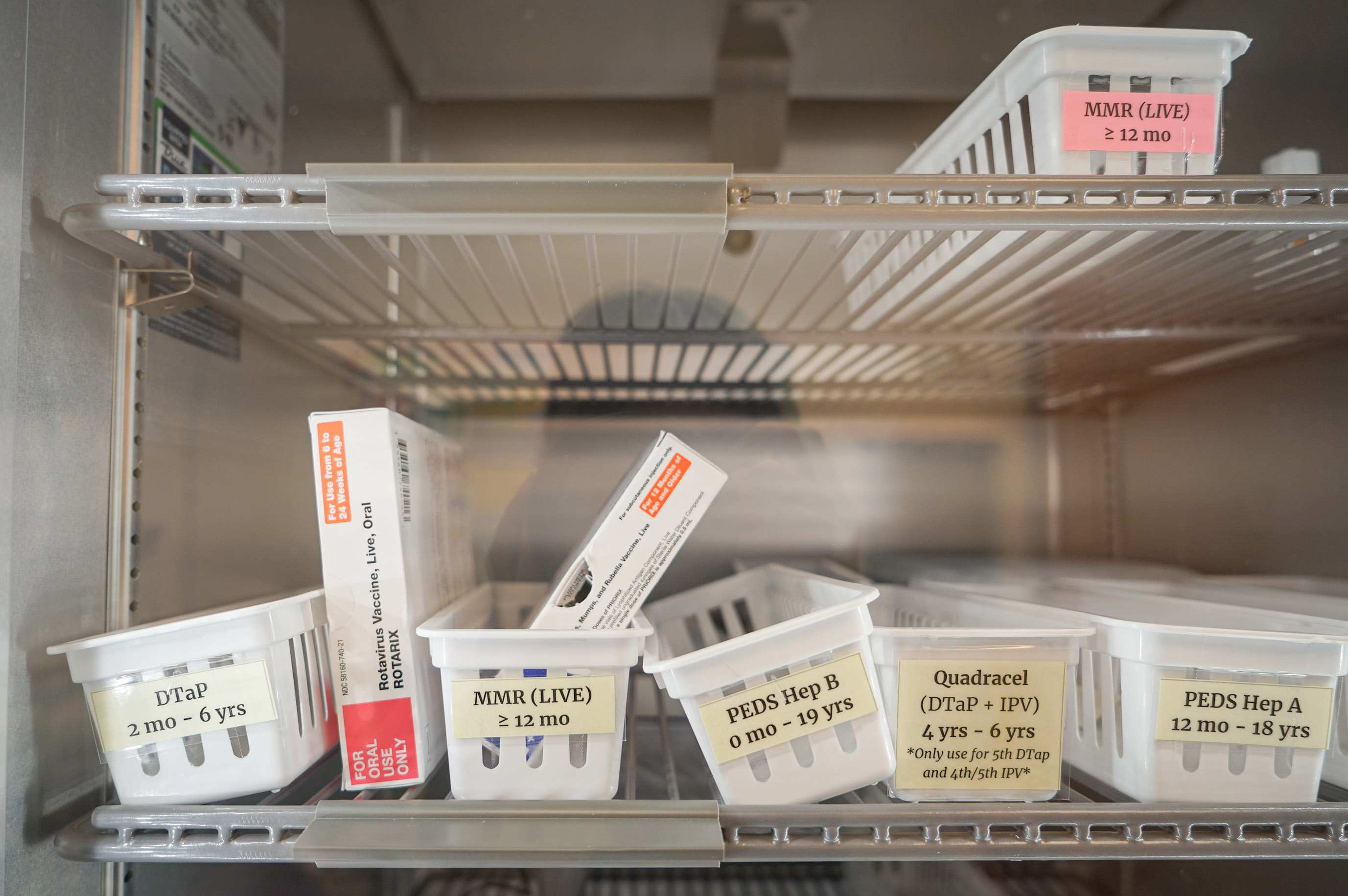
In communities nestled among the red sandstone cliffs and riparian forests of southern Utah, measles took hold last summer. At the main school in Hildale, a town along the Arizona border, just 30% of kindergartners are considered adequately immunized by Utah’s health department, meaning they’ve gotten recommended vaccines against measles, tetanus, polio, and more. Exemptions from childhood vaccine requirements are easily acquired in the state: Parents need only claim personal, religious, or medical reasons.
Many people in Hildale and the surrounding towns are connected to the Fundamentalist Church of Jesus Christ of Latter-Day Saints, a sect that has been leery of the government since a police raid in 1953 separated polygamous parents from their children. Shirlee Draper, a southern Utah resident who grew up in the faith, said they became ever more isolated in the early 2000s under the leadership of Warren Jeffs. Before he was sentenced to life in prison for sexual assault against minors, Jeffs instructed his followers to withdraw from public schools and mainstream medicine.
“Growing up, we all got our vaccines,” said Draper, who left the group during Jeffs’ reign. “It wasn’t until Warren Jeffs came along that there started to be more and more resistance.”
After Jeffs went to prison, many people left the faith but remained concerned about vaccines because of online misinformation, such as claims that the shots are toxic. Today a small shop in Hildale sells mouth sprays and oral drops professing to detoxify vaccines. Water, glycerin, and “whole grain alcohol” are listed as ingredients in one called Vxx-Dtx.
A mother who KFF Health News agreed not to name, because she fears stigmatization, said she considered getting her kids vaccinated when schools in southwest Utah started seeing measles cases last summer. She had split from the fundamentalist group but still worried about vaccines giving her children autism or other complications. Large studies published in top-tier scientific journals have refuted a link between vaccines and autism, but the anti-vaccine movement has kept the notion alive.
Then the woman’s son told her that his classmate had a rash and spit on him, she said. A few days later, he fell ill with a fever, followed by vomiting, diarrhea, and a head-to-toe rash.
“He felt downright sick for 10 to 14 days,” the woman said. “It was hard to see the end of the tunnel.”
Then her daughters came down with measles. She had a fleeting case, too, even though she had been vaccinated as a child. Breakthrough infections tend to be mild and are relatively rare. Only 4% of 4,300-plus U.S. cases reported this year and last have been people who’ve had two doses of the measles, mumps and rubella vaccine.
By the time the family recovered, the son had missed nearly three weeks of school, the daughters a month, and the mother had postponed an important family gathering because she didn’t want to spread infections. “I just got my youngest’s missed-school report and it’s super high,” she said. “This is the year of sickness.”
The woman said she regretted not getting her kids vaccinated when the outbreak started. She said she knows about 30 people who have fallen sick with the measles. Except for a few who needed medical care, they haven’t been tested. “I bet there’s been thousands of cases,” she said.
Measles doesn’t have a cure. She and others have tried to ease symptoms with cod liver oil, vitamin C, zinc, and “essential oils,” plant extracts long used in folk medicine that have become a lucrative industry in Utah. People in southwest Utah are trying a lot of things: One resident sells homemade lotion on Facebook, writing, “Breastmilk & Honey has been a life saver for the measles rash.”
Beyond Containment
The outbreak may have started among a fundamentalist community, but it’s spread far beyond because Utah’s vaccination rates have dropped steadily since the covid pandemic. Fewer than 80% of kindergartners were adequately immunized in the 2024-25 school year in southwest Utah, with only 87% adequately immunized in the state as a whole — far below the 95% threshold required for herd immunity.
Several Utahns told KFF Health News that “alternative health” or “wellness” drives the trend, rather than religion. The state has a thriving supplement industry, worth $6.1 billion in 2023, aided by deregulatory policies supported by the late Utah senator Orrin Hatch and a high concentration of people who earn income from multilevel marketing. These networks of people sell supplements, essential oils, peptides, and other alternative therapies on social media, YouTube, and podcasts, according to scholarly articles and industry analyses.
Alternative health isn’t necessarily anti-vaccine, but many people who sell unconventional remedies online and in podcasts deride vaccines and mainstream medicine.
“People are suspicious, and it’s well founded,” Draper said. She described dismissive doctors, exorbitant medical bills, hospital systems that put profits over care, and pharmaceutical companies that drove opioid addiction. Communities already wary of government authorities are poised to interpret failings in American healthcare as signs that medical authorities aren’t to be trusted, either, she said.
“Across America, we have entire populations who find safety in clinging to whatever confirms their deeply held beliefs,” she said.
A mistrustful disposition gave way to covid conspiracy theories in 2020 and 2021. In southwest Utah, for example, a pickup truck tricked out with digital billboards showed up to covid vaccination sites to advertise Plandemic, a 26-minute viral video rife with conspiratorial claims, including that masks “activate” the coronavirus and that global elites planned covid-19 to control the population. Misinformation added fuel to anger about public health rules, and there was political backlash under the umbrella of a largely Republican “medical freedom” movement. Utah enacted laws reining in public health, including one that eases exemptions to childhood vaccinations and another that prohibits most employers from requiring vaccines.
In the wake of the covid backlash, health officials tread lightly. Rather than enforce containment measures, “we give our advice and focus on personal responsibility,” said David Heaton, public information officer at the Southwest Utah Public Health Department.

One of the most contagious diseases in the world, measles spreads with astonishing speed among the unvaccinated. One meticulous study of a New York school outbreak in 1974 found that a second-grader with measles infected 28 other students in 14 classrooms because measles can spread through ventilation systems.
As cases doubled then quadrupled in southern Utah, the regional health department couldn’t keep up with calling the contacts of everyone infected. It shifted its efforts to announcements guiding the public at large. For example, it asks people to call before showing up to clinics with measles symptoms. Still, patients in plenty of hospitals have been exposed. For example, when parents brought a sick, unvaccinated child to a large pediatric hospital in Utah in September, they shared the space with 11 infants too young to be vaccinated. Doctors rushed to give the babies infusions of antibodies and they remained healthy, according to a recent report.
On the radio and in posts on social media, Heaton warns that measles is spreading and that vaccines are the best defense. “If you’re not immunized and you’re anywhere in public,” Heaton said, “you’re fair game for this virus.”
The department doesn’t have the capacity to talk with people directly in the five counties it serves. For a few years, it leaned on community health workers who went to churches, town halls, and other gathering places, listening to people’s concerns and telling them what the science said about covid, vaccines, and other matters of public health. But these workers were laid off early last year, after the Trump administration clawed back more than $12 billion in federal public health grants to states.
“We were starting to get a little bit of traction,” Heaton said of the community workers. “And then we lost all of our team.”
The department offers free measles vaccines to children, but uptake is slow. Nursing director Mindy Bundy said that when she started the job 20 years ago, demand was so high that she would give parents tickets while they waited, as if they were crowding around a deli counter.
“Now even in an outbreak,” she said, “we aren’t seeing a huge increase of people wanting vaccination.”

As officials tried to do the best they could, the outbreak spread north, hopping from one undervaccinated community to the next. When health officials in Utah County spoke with people who had tested positive, they often had no connection to other known cases. “Pretty quickly, we started to lose the links,” said Michael Leman, the county health department’s nursing director. Contact tracing, the cornerstone of containment, was failing.
Every week, the state health department posted a growing list of locations on its website — a Trader Joe’s, a Mormon temple, an aquarium, preschools — that people had visited while contagious. But many people who tested positive hadn’t been to those places, Leman said. “They could have gotten it at Walmart. They could have gotten it walking through a mall,” he said. “I mean, just anywhere in the public they could have been exposed.”
In February, high school students throughout Utah tested positive after a state wrestling tournament at Utah Valley University in Orem. A dashboard monitoring measles viruses in wastewater lit up with notifications around the state. “Wrestling really feels like our turning point,” said Nicholas Rupp, communications director at the Salt Lake County Health Department.




Salt Lake County’s shift from containment to mitigation meant prioritizing high-risk situations and relaxing control everywhere else. When a student has a confirmed case, for example, health officials meet with the school nurse to figure out which kids are most vulnerable. Unvaccinated children in the same classroom as someone infected are asked to stay home for 21 days, but those in other classrooms might not be, said Melanie Crossland, an epidemiologist at the Salt Lake health department. Some schools with high vaccination rates have opted to monitor student temperatures daily instead of requesting quarantines. One school created a separate space for the unvaccinated.
Crossland said such bespoke strategies entail a “huge” amount of effort but have staved off blowback that deflated her during covid.
“We give everything when we’re here,” she said, “but the days of killing ourselves, when legislatively no one is going to give us any help, are done.”
Daycare Dilemma
The outbreak has lasted so long that some children who have recovered from measles have since been hospitalized for what should be mild illnesses from common bugs, said Kerri Smith, a hospital pediatrician in southwest Utah. Measles can erase the immune system’s memory, impairing a body’s ability to fight other viruses. “It’s making children very susceptible to getting sick again,” Smith said.
Her eyes were bloodshot, and she looked drained from a week of long shifts. Since the outbreak began, she’s treated more than a dozen babies and children severely sick from measles.
“They’re usually admitted to the hospital with measles pneumonia, so they’re struggling to breathe, pulling for air below their ribs,” she said. “High fevers, 104 to 105, absolutely miserable, extremely fatigued, really dehydrated with sunken eyes.” Most children fully recover from measles, but a fraction develop permanent hearing loss, a small percentage die, and in rare cases, measles kills a person years after the infection.
No one has died so far in Utah’s outbreak. And barring that tragic outcome, Smith and other doctors said, some parents fail to grasp the gravity of measles, even as their own children have tubes inserted into their small nostrils to deliver oxygen. Despite repeated warnings, doctors said, some unvaccinated family members of patients — who could be contagious — walk around the hospital while visiting their loved one. This means the waiting room, the elevator, the cafeteria, and other places need to be shut down for cleaning, and vulnerable people alerted.
“People don’t realize how easily this spreads,” Smith said.
Morris, the pediatrician working in two counties, recalled a conversation with a nonchalant father who didn’t seem to understand the need for quarantine. “I know this is an inconvenience to you,” she said. “It’s also a huge inconvenience to the parent who has an infant who could be severely impacted by this disease.”
On top of feeling depleted, doctors with young children said they are anxious. Emily Chin, a physician in Salt Lake County, worries she’ll bring measles home to her newborn. One evening, she sat in her garage after caring for a child with a rash. The patient’s measles test was still being processed, so Chin isolated herself in a room for the night, wearing an N95 mask instead of holding her infant.

Like many mothers in Utah, Chin plans to give her baby an early dose of the measles vaccine at 6 months old because of the outbreak, in addition to two doses at ages 1 and 4. Several mothers said they avoid travel and public places because they fear their babies could be infected. Some are delaying daycare. Others, like Kandace Hyland, a marketing director in Salt Lake County, don’t have that option.
Hyland was shocked when her daycare told her that it didn’t track the vaccine status of staff, even amid the outbreak. In March, she posted an online petition calling for the state to require daycare staff to be vaccinated against the measles when the virus is spreading. Even if daycare staff file for vaccine exemptions, she said, parents could at least find out what portion of their babies’ caretakers pose a life-threatening risk.
Hyland sent her idea to the state health department. Nolen, the state epidemiologist, said she agreed with the concern, and was “talking with the division of licensing about the issue,” in an email shared with KFF Health News. Hyland also wrote the Division of Licensing and Background Checks. In an email, its director, Shannon Thoman-Black, replied that the division does “not have the legislative authority to implement a mandate.”
“They always talk about parents’ choice,” Hyland said. “But I don’t feel like I have a really good ‘parents’ choice’ right now.”
Measles’ Comeback
The U.S. will almost certainly lose its measles elimination status this year or next, but it could be regained if political leadership backed nationwide campaigns to boost confidence in vaccines, said Demetre Daskalakis, a former director of the Centers for Disease Control and Prevention’s national immunization center and now the chief medical officer at the Callen-Lorde community health center in New York.
“Under Secretary Kennedy’s leadership, that’s unlikely to happen,” he said. “We’re going back to a pre-vaccine era.”

HHS spokesperson Emily Hilliard defended the secretary and his agency in an email, writing that the CDC has “surged resources” to contain measles outbreaks. “The CDC, HHS principles and the Secretary have been vocal that the MMR vaccine is the best way to protect yourself against measles,” she said.
Kennedy’s words and actions suggest otherwise. He’s said that the measles vaccine leads to “deaths every year,” which is not true. He continues to tout a potential link between autism and vaccines, no matter how many studies conclude there is none. And he oversaw abrupt changes to the recommended childhood vaccine schedule, a move medical societies called dangerous and not backed by science. A federal judge blocked those changes in March, but Trump recently issued an executive order to reexamine the schedule.
“It’s been confusing for the public,” said Dorothy Adams, executive director of the Salt Lake County Health Department.
In May, Kennedy met with Republican Utah Gov. Spencer Cox, who has said little about the state’s ongoing outbreak. Kennedy praised Utah’s action on Make America Healthy Again priorities, such as banning fluoride in public drinking water and easing restrictions on raw milk sales, according to Salt Lake City’s Deseret News. Cox declined to comment for this article.
Meanwhile, the chronically depleted U.S. public health system has been further weakened by the Trump administration’s cuts and delays to public health grants.
“If you’re in the thick of it and you don’t know if you will be reimbursed, you adjust your response,” said Angela Dunn, a doctor and former Utah state epidemiologist. “This outbreak is a perfect storm of disinformation, trauma from the covid pandemic, and the drop in funding.”
Measles isn’t the only preventable malady making a comeback. As children played nearby in a sun-speckled park in Salt Lake City, Morris talked about a baby in the intensive care unit who was bleeding uncontrollably after a fall. The baby’s parents had refused an injection of vitamin K that helps blood clot in newborns. As they fretted over their infant, Morris said, she felt awful for them and regretted not being able to overcome mistrust in basic, lifesaving interventions. She had the same swirl of emotions when an unvaccinated toddler in her care recently died of whooping cough.
“I was one of the only people in the room with the nurse when the child coded,” she said with tears in her eyes. “You think, ‘I wish this child was vaccinated,’ but it’s hard because I also see how much grief these parents are holding.”
This <a target="_blank" href="https://kffhealthnews.org/public-health/utah-measles-outbreak-vaccines-preventable-diseases-doctors-strained-new-normal/">article</a> first appeared on <a target="_blank" href="https://kffhealthnews.org">KFF Health News</a> and is republished here under a <a target="_blank" href="https://creativecommons.org/licenses/by-nc-nd/4.0/">Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="https://kffhealthnews.org/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="https://kffhealthnews.org/?republication-pixel=true&post=2248142&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">from KFF Health News https://ift.tt/eYvnXyi





 Rose
Rose